Like so many people afflicted by the pandemic, Albert Palmares could not visit his mother while she was hospitalized for COVID-19. As facilities like Weill Cornell Medical Center tightened their safety precautions to slow the spread of COVID-19, Palmares and other families felt the anguish of isolation as their relatives fought a debilitating disease alone.
Although modern technology offers some contact-free communication, phone calls and video chats come with limitations in a hospital setting. “The only way I could talk to my mom was via iPads when the nurses were available to help,” says Palmares, a medical student studying in the Philippines, who called the hospital every day to ask if a nurse would hold up an iPad so that he could chat with his mom. “This just added more responsibilities for the nurses who were busy taking care of patients.”
When Palmares returned to the U.S. to support his mom’s recovery, he learned about Weill Cornell’s new VoiceLove Project, which enabled him to speak directly to his mother anytime, from anywhere, using an app that relayed real-time messages to a small walkie-talkie-style device installed at her bedside in the intensive care unit (ICU). If she was up to it, his mother could also respond by simply pushing a button on the screenless device, which was originally designed as a safe, easy alternative for parents to stay in touch with their children. The simple technology allowed Palmares and other families to talk to immobilized ICU patients without staff intervention. “Using the device to communicate with her was valuable to our whole family,” Palmares says. “It gave us hope and peace of mind that she’d hang on to our words and pull through.”
Palmares heard about the VoiceLove Project from Marc H. Schiffman, MD, an interventional radiologist at Weill Cornell who developed the initiative with gynecologic surgeon Tamatha B. Fenster, MD, MS, to help alleviate constrained communication between stressed medical staff and concerned families coping with COVID-19. By leveraging the walkie-talkie-style devices to solve a multidimensional clinical problem, the VoiceLove Project has made a powerful impact on patient care during the pandemic.

To help ICU physicians during the COVID-19 pandemic, gynecologic surgeon Tamatha B. Fenster, MD, MS, and interventional radiologist Marc H. Schiffman, MD, spearheaded the VoiceLove Project to keep families connected to patients in isolated care at Weill Cornell. |
“Even though we can’t control the pandemic, the one thing we could control was communication — bringing humanity into a sad situation by allowing families to stay connected during a traumatic time,” Fenster says. “There’s no reason to let people suffer from separation and lack of communication when we have access to such a simple technology to fix the problem.”
Seeing a Critical Communication Strain
When COVID-19 cases began surging in New York City by April of 2020, Fenster volunteered to help in Weill Cornell’s busy ICU. She was ready to report for duty, but because so many physicians across the state offered their aid, the ICU no longer needed her medical assistance. With “a burning desire to help in the height of the pandemic,” Fenster began looking for ways to offer non-clinical support instead.
She heard the hospital’s morning report one day, highlighting how physicians in Weill Cornell’s pop-up ICUs were trying to provide patients’ families with daily updates since the virus had halted visitation. Realizing the challenge of balancing communication with critical care, Fenster conceived the idea to act as a liaison between strained medical staff and families desperate to connect with their loved ones in the ICU.
Fenster called Schiffman, a longtime friend and colleague, and asked him to join a virtual meeting with other attending physicians, nurses, and social workers stationed in the ICU. During the call, Fenster proposed a program called Critical Care Connect, in which she and other volunteers would accompany inundated ICU teams on daily rounds and then call each patient’s families with status updates.
The physicians were relieved to have help, and Schiffman and Fenster began rounding with an ICU team the next day, on Saturday, April 18. As soon as they started making calls, they realized that families wanted more than a brief medical update. “We found that the families didn’t really care about the blood pressure or other medical minutia that we thought was important to share,” Fenster says. “They just wanted to talk to their loved ones. They wanted human connection.”
Recognizing that telephone updates weren’t providing the level of interaction that families craved, medical professionals had been using the FaceTime app on iPads to let family members like Palmares communicate with patients in isolated care. Schiffman and Fenster tried to facilitate these video chats as part of Critical Care Connect, but the challenges piled up quickly.
The video experience made some families uncomfortable. “Their loved ones, who looked healthy just a few weeks ago, were now intubated and hooked up to ventilators,” Fenster says. “That can be a distressing sight to see, so it didn’t give the families solace.”
Call coordination presented other obstacles because it required time and personal protective equipment (PPE) when medical providers didn’t have much to spare. “During the COVID-19 surge, patients’ families commonly asked us to hold up an iPhone or iPad so that patients could hear their voices,” says Christine Lennon, MD, an anesthesiologist working in a pop-up respiratory ICU at Weill Cornell. “We tried to accommodate these requests when possible, but every time we entered a patient’s room, we had to fully don PPE, which was in short supply. We had to minimize the risk of exposure to the staff while also being mindful of PPE utilization. We had to weigh the emotional needs of our patients and their families against the time and resources required to facilitate these calls.”
Schiffman and Fenster quickly noticed that families were desperate to contact COVID-19 patients beyond the daily medical updates, but they needed a way to communicate without putting the nurses and physicians at increased risk of exposure. “We couldn’t justify using additional PPE just to hold up an iPad for each patient, especially when these brief calls weren’t really helping families,” Schiffman said. “We knew there had to be a better way.”
Brainstorming Better Tools
Recognizing that the hospital desperately needed a more efficient mode of connecting families with patients in the ICU, Schiffman and Fenster immediately began brainstorming options for contact-free communication. They toyed with the idea of walkie-talkies, which could affordably enable two-way conversation, but they would have required coordination to distribute the devices. After searching Google for walkie-talkie alternatives, they discovered Relay — a small, simple push-to-talk speaker that sends and receives messages through a coordinating smartphone app.
After his shift one Saturday night, Schiffman drove to a Target store in Harlem and purchased two Relay devices, which retail for about $50 each. The next morning, after rounding with the ICU team, he began calling families and asking if they wanted to speak to their relatives in the ICU by downloading the app to convey a message through the speaker placed by the patient’s bedside.

A small hands-free speaker mounted to a patient’s bedside relays messages sent from family members anywhere in the world, using an app-based walkie-talkie technology designed to let parents contact children without a smartphone. |
“The first few families who tried it were so grateful and relieved to finally speak to their loved ones,” he recalls. “Instead of waiting around by the phone all day, desperate to get a call from the hospital, families could use the Relay app anytime, from anywhere in the world, to broadcast a message directly into the patient’s room. As soon as we tried it, we knew we were on the right track.”
To expand this effort, Schiffman knew they’d need more devices. That afternoon, he contacted Relay’s executives, who agreed to donate enough devices for all of the patients on ventilators at Weill Cornell. They even waived the device’s standard monthly subscription fee and streamlined the app interface so that patients’ families could simply open the app and push a button to talk, without entering personal details or billing information.
Later that evening, Schiffman and Fenster emailed their respective department chiefs, explaining their idea to deploy these devices to connect families with patients isolated in the ICU. With their support, Schiffman and Fenster then emailed the hospital’s chief operating officer, who scheduled a videoconference the next morning to discuss their plans for administering the program. “We knew that if we were going to approach the highest levels of hospital administration to green-light this idea, we’d need a complete proposal that addressed the problems we saw in the ICU and the solutions this device offered,” Fenster says. “As a bonus, the hospital could deploy the devices free of charge.”
After the IT team spent a few days evaluating the software for patient privacy and compliance, Schiffman and Fenster received the final sign-offs to launch the initiative within one week of proposing the idea. “The solution had to be immediate,” Schiffman explains. “It was really to the credit of the Relay executives and the hospital administrators who responded so quickly to move this idea forward. Everyone knew that if we didn’t act fast, people were going to miss their chance to say goodbye to their relatives in isolated care.”
Translating Tech to a Medical Setting
Schiffman and Fenster gradually began deploying more Relay devices in the busiest ICU at Weill Cornell. Within a few weeks, they had distributed about 15 devices across two units. Although the ICU nurses were nearly as relieved as the families to have a hands-free communication option, the staff quickly observed a few limitations of the device.
First, they noticed that the sticky-note-sized device was difficult to place in ICU rooms, where people and equipment moved around frequently. “When you moved the bed, the device would fall to the ground, and the plug kept getting disconnected,” Fenster explains. “The whole idea is to be hands-free. If the nurse has to keep plugging it in, it defeats the purpose.”
Another feature that made nurses nervous was the button in the center of the Relay speaker that, when pressed, could send messages in response. “In a hospital setting, any device that has the suggestion of two-way communication can be a little bit unnerving,” Fenster says, “because you don’t want to accidentally press the button or broadcast private information.”
The nurses also worried that the tiny holes in the speakers couldn’t be thoroughly disinfected, potentially posing risks for cross-contamination. As these concerns mounted, Fenster and Schiffman began brainstorming again to adapt the consumer device for the medical setting. “We started sketching a case to hold the speaker,” Fenster says. “We came up with a clamshell case that allowed the device to be Velcroed to a bedrail or wheelchair and offered a protective cover that prevented the button from being accidentally pressed and eliminated any cross-contamination. If the case did get soiled, you could just discard it and get a new one.”
Fenster contacted an industrial designer she knew from college to bring their sketches to life. He volunteered his time to 3-D print a prototype case that addressed all of the nurses’ concerns about the speaker. Fenster and Schiffman began ordering cases from several local factories, then driving from Brooklyn to New Jersey to pick up the products.

To make Relay’s off-the-shelf consumer device appropriate for medical settings, Schiffman and Fenster had a plastic case designed to protect the small speaker from cross-contamination. |
To mass-produce cases more quickly, they decided to vacuum-mold 1,000 PVC plastic shells through a supplier overseas. Though the production costs quickly added up, Fenster and Schiffman were committed to giving back during the pandemic and covered the costs out of their own pockets.
The cases turned the program into a home run, formalizing the VoiceLove Project around mid-May of 2020. By the time the cases were produced, the effort had already grown to deploy 40 devices across four ICUs at Weill Cornell, helping families send patients nearly 12,000 messages totaling 3,000 minutes.
Building Buy-In
Although Schiffman and Fenster hoped to expand the initiative as fast as possible, they wanted to ensure they rolled it out properly. To that end, they developed a thorough process to onboard ICU teams unit by unit.
To start, they scheduled videoconferences with nursing directors and senior social workers, who decided which individual units could benefit most from the program based on the volume of requests from families calling frequently to connect with COVID-19 patients. Then, Schiffman and Fenster coordinated in-service training for each unit’s team. “Anytime you’re introducing something novel in a hospital, it’s a challenge because you have to explain that it will actually simplify their job, not add more work,” Fenster says. For that reason, they kept the training quick and simple.
The 15-minute training consisted of a five-minute video that explained the VoiceLove Project, a live demonstration showing how to attach and use the device, and a short PowerPoint that shared testimonials from staff and families who had used it.
The key to building buy-in from each unit was winning over the social workers, who were responsible for explaining the program to families. Fenster and Schiffman equipped them to introduce VoiceLove with simple, three-step instructions that walked families through downloading the app, logging in, and pushing a button to send a message.
“As social workers, we weren’t allowed to go into COVID-19 rooms because of limited PPE. We felt so helpless, and the families felt so disconnected,” says Avery Ornstein, LCSW, a senior social worker at Weill Cornell who covered the ICU during the pandemic. “Having this program was such an amazing link to connect families and bridge this gap by giving them direct access to their loved ones.”
After helping families set up the app, social workers gave the Relay device to a nurse, who would hang the speaker by the patient’s bedside while they were checking vitals or administering medication. The easy installation fit into existing workflows, saving nurses from using precious time or extra PPE. “The VoiceLove Project allowed us to focus our energies on delivering medical care,” Lennon says. “During the COVID-19 surge, a lot of us were operating at maximum capacity, so relieving that one burden of family communication really made a big difference.”
Improving Patient Care
Many patients’ families referred to VoiceLove as a lifeline to their loved ones in the ICU. Without depending on the availability of busy nurses, people like Palmares could use the device to send messages, prayers, songs, and other spontaneous updates whenever they wanted. “Relatives from around the globe were chiming in to encourage and pray for my mom,” Palmares remembers. “It was therapeutic for us, and hopefully also for her, to have that connection when we couldn’t visit her.”
The app works with cellular networks and Wi-Fi to provide unlimited range, allowing family members access from anywhere in the world. “The VoiceLove device enabled multiple family members to communicate freely without feeling like they were burdening the medical staff,” Lennon says. “This program helped relieve that feeling of guilt they felt for taking additional time from medical teams that were already stretched thin.”
Most importantly, the VoiceLove Project gave power back to patients’ families during the pandemic. “What this program provided — more than communication, more than connection — was control,” Fenster says. “It provided a sense of empowerment in a situation where people felt helpless. It allowed them to reach out to their family member on their own timeline, whenever they wanted to tell their dad they loved him. It gave them back the control over communication that they were completely robbed of during COVID-19.”
As much as families appreciated this unlimited access, certain reactions suggest that patients benefited just as much from the exchange. “The first time I set up a VoiceLove device for one of my patients, his daughter said prayers in his native language,” Lennon recalls. “I could see that he recognized her voice, and his demeanor distinctly brightened in that moment.”
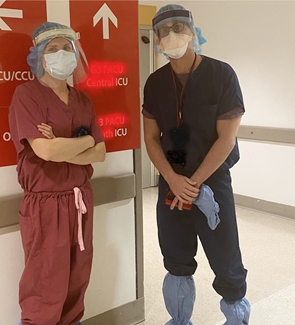
With a limited supply of PPE, Weill Cornell physicians Tamatha B. Fenster, MD, MS, and Marc H. Schiffman, MD, leveraged hands-free walkie-talkie devices to let families speak to COVID-19 patients in the ICU without putting medical teams at risk of exposure. |
Schiffman saw countless examples of positive responses like this, even from patients under sedation. “One patient in particular had not shown much mental status, and discussions had begun about withdrawing care,” he says. “But about 10 minutes after hooking up the device, when his grandchild’s voice popped over the speaker, his eyes moved. In the following days, every time another family member spoke, you’d see a facial expression or a tear in his eye. We saw obvious changes happening after hearing the family’s voices — making it evidently clear that this was making a difference for patients.”
Some
research suggests that family presence and participation can reduce ICU patients’ psychological stress and potentially aid in recovery. Schiffman and Fenster are currently applying for grants to study the program’s impact on comatose patients. “We should do everything we can to maximize family participation in this unprecedented situation of social isolation,” Lennon says. “There are real benefits to the patients’ medical outcomes when they have the emotional support of their loved ones.”
Innovating Beyond the Pandemic
Six months after launching the VoiceLove Project in April, Schiffman and Fenster had deployed more than 160 donated Relay devices throughout 11 units at Weill Cornell. As more nurses, social workers, and families heard about the walkie-talkie devices being used to connect with COVID-19 patients, they requested access.
These requests gradually expanded the initiative beyond the ICU into palliative care units, where families were desperate to speak to their relatives one last time before withdrawing care. “Families have repeatedly said that this experience is going to give them comfort for the rest of their lives,” Schiffman says.
Even though hospital visitation slowly reopened at Weill Cornell in early June to allow one visitor per patient, the devices are still being widely used. Social workers are starting to administer the in-service training for new units, as Fenster and Schiffman develop plans to deploy the program at other hospitals in their network.
“We see innumerable applications for this device to continue to connect patients with their families — not just during the pandemic, but afterwards,” says Schiffman, suggesting that radiology patients could use the VoiceLove devices when they don’t have cell phone access or reception while waiting for exams. In neonatal ICUs, mothers could use the devices to sing to their newborn babies before holding them. Likewise, the device could connect families with patients in pre-op and post-op settings with limited physical visitation.
Although an interventional radiologist and a gynecologic surgeon might seem like an unlikely pair to spearhead an urgent communication initiative, Schiffman points out that radiologists are known for constantly applying new technologies to medicine.
“Technology is going to drive a lot of change in medicine going forward, and as radiologists, we’re in a unique position to pioneer technical innovations that can really improve patient care,” he says. “Not all medical technologies have to be designed specifically for a hospital. By adapting this simple existing technology to work in a hospital setting, we’re helping people stay connected in the short-term and reshaping hospital communication over the long-term.”
If you would like to obtain VoiceLove for your hospital, please email: voicelovedoctors@gmail.com





