A radiologist-led 3D-printing lab produces personalized models to guide surgeries and enhance patient care.
- The University of Cincinnati recruited a leadership-based radiologist with medical 3D printing experience to develop a 3D-printing lab with a team made up of trainees, radiologists, engineers, and surgeons.
- The 3D printed anatomic models help guide complex procedures, advancing endoscopic surgery opportunities as well as providing educational tools for medical trainees and patients.
- Although 3D printing has been performed in healthcare facilities for over a decade, it continues to expand. As an example, 3D printing and digital surgical planning guided the first endoscopic cardiac triple valve repair surgery in the U.S. in 2021.
In June of 2021, a patient was admitted to the intensive care unit at the University of Cincinnati (UC) Medical Center with severe cardiac triple valve (aortic, mitral, and tricuspid) disease, and subsequent heart failure. World-renowned cardiovascular surgeon Tommaso Hinna Danesi, MD, worried about the patient’s prognosis. The patient desperately needed an intervention but was too frail for open heart surgery. “The only surgical option I could offer her was an endoscopic one,” says Hinna Danesi, associate professor of surgery at the UC College of Medicine. “Like triple valve disease, an endoscopic operation of this nature is incredibly rare.”
Hinna Danesi is one of only a dozen surgeons worldwide who perform endoscopic multi-valve heart surgery. Before joining the UC Medical Center in March of 2021, he had successfully conducted the procedure in cases involving one and two valves in his native Italy, but he knew that accessing three valves through one small incision would be difficult.
“Heart valve location varies among patients, and in the diseased heart it is even more unpredictable. You cannot access all four valves from one unique site on the chest without a thorough understanding of the patient’s anatomy,” Hinna Danesi explains. “The access point for the aortic valve, for instance, is different from the one for the mitral, tricuspid, and pulmonic valves.” Thanks to innovations in UC Medical Center’s radiology department, Hinna Danesi could approach the surgery more prepared than ever before.
Several years earlier, Frank J. Rybicki, MD, PhD, vice chair of imaging operations and quality in at UC Medical Center, established the department’s 3D-printing section. The clinical service uses CT and MR images to create personalized medicine via anatomic models, anatomic guides, and digital surgical planning. The anatomic models allow surgeons, like Hinna Danesi, to plan and even practice their procedures.
“The surgeons can hold the model and understand the patient’s anatomy in a unique way. In doing so, the tactile feedback and insights from the true depth perception equips them with unprecedented insights to the pre-operative anatomy, before they get in the operating room,” explains Rybicki, who is also co-chair of the ACR 3D Printing Registry Governance Committee and a member of the ACR Commission on Economics. “Our providers also share the models with their patients for education and con-sent. The patients always come away more informed.”
“The more I thought about it, the more applications I saw for this technology. For instance, I envisioned patient-specific 3D-printed guides for more accurate placement of radiation seeds in patients with a post-surgical deformity,” Mahoney says. “I got excited about it, and the literature supported my instincts that radiology is becoming more patient-centric and 3D printing is the best way to carry that into the future for Cincinnati and as a profession.”
Mahoney’s instincts were confirmed and amplified when she spoke with surgeons and other physicians during tumor boards who found value in patient-specific 3D-printed models. They shared a range of scenarios in which the models would be useful, including, for instance, pelvis fracture, tumor resection, and cardiothoracic procedure planning, all of which are notoriously complex. Knowing that the surgeons would use the models, Mahoney committed departmental budget to launch a new 3D-printing clinical service and recruited Rybicki, a globally recognized leader in the field, who in 2011 developed 3D models to guide the nation’s first full face transplant at Brigham and Women’s Hospital. Rybicki was chair of radiology at the University of Ottawa Department of Radiology and the Ottawa Hospital in Ontario, Canada, at the time that Mahoney began recruiting him.
“I was well aware of Frankie’s work because it had received so much attention in the media and the radiology world, particularly his work on the face transplant. We had also known each other years before as we both worked on the ACR Committee on Appropriateness Criteria,” Mahoney says. “His name surfaced again when a former colleague of mine who co-launched the renowned 3D-printing section at the Mayo Clinic Rochester, Jane Masumoto, mentioned that Frankie might be able to launch and lead our program. I got in touch with him and that’s how it all began.”
In outfitting the lab, Rybicki considered two types of desktop printers, each of which uses a different printing method. One is called vat polymerization and the second is called material extrusion. Vat polymerization printers use ultraviolet light that converts a vat of polymer resin into a physical 3D-printed model. Material extrusion printers share similarities with glue guns; they dispense one or more heated polymers through a printer head and onto a build plate, depositing each successive two-dimensional layer to create the 3D-printed part. “Schools and universities commonly use these two types of printers,” Rybicki explains.
Rybicki initially setup the printing lab in a vacant room within the radiology department. But he and the trainees were inundated with requests for models, and the group needed more room for a second printer and space with good ventilation to control the strong fumes that 3D printing produces. Recognizing the growth in the clinical service, Mahoney saw an opportunity to move the lab into a new space that was created as part of an already planned departmental renovation project. The new space includes a negative air pressure system, space for sterile operations, and proper desktops and water facilities for a mid-sized 3D-printing lab within a medical center.
Now, when a surgeon, interventional radiologist, or cardiologist orders a model through the electronic health record, Rybicki reviews the images and then meets with the ordering physician to review the case. As a result, he has forged relationships with over a dozen providers who are integral to the success of the clinical service itself. “I always perform a detailed consultation with the ordering physician,” Rybicki says. “I’ll call the provider and ask them for the intended use of the model and how we can deliver quality for the lowest possible cost. At this point, my relationship with providers is quite strong, but each time we tackle a unique problem there is a healthy back and forth about what we’re trying to achieve.”
With the help of an engineer, Rybicki will then segment the patient’s MRI or CT images to create a digital blueprint of the model. He also transfers the imaging information from the digital imaging and communications in medicine file format to a stereolithography file format. “Printing a model includes translating the imaging data from radiology language into manufacturing language so that the 3D printer can recognize it,” Rybicki explains. “Then we send that information to the printer to create the model, a process that can take between six to as many as 30 hours.”
Given the time and cost associated with printing a model, the team makes them for only complex cases. Once a model is completed, Rybicki meets with the surgeon again to review the model. From there, the surgeon can use the model to better understand the anatomy before entering the operating room. The surgeon will often practice on it. “They might drill or cut through the model as they’re deciding how to access a brain tumor, for example,” Rybicki explains. “Occasionally, the surgeon will sterilize the model and take it into the operating room as reference. It’s a game changer for surgeons, and they continue to ask for it.”
In addition to using the models to plan procedures, Hinna Danesi often shares the models with patients to help them understand their complex cases. While the models are likely easier for patients to understand than radiology images, Hinna Danesi says they’re still not completely intuitive to the untrained eye. “A non-medical person can understand the ribs and the chest cage, but they cannot really understand the anatomical structures behind them because they usually are not colored or intricately detailed. The technology is still in its infancy,” Hinna Danesi explains. “But some patients are very curious, and they want to go deep into the procedure and how we plan everything, so I usually take time to show them their model.”
While the lab started out creating models for surgical planning, Rybicki and his team recently expanded its scope. The clinical service now creates personalized surgical guides for craniomaxillofacial reconstruction. For example, if a patient loses part of their jaw from a tumor or trauma, the team can use imaging to map the exact shape of the void. From there, they can 3D print a guide that the surgeon can use to more precisely reconstruct that part of the bone and the necessary blood supply for a successful procedure. “The guides are like cookie cutters that the surgeons can use to cut the bone, and it will be the perfect size and shape with all of the blood vessels intact,” Rybicki says. “It significantly reduces the amount of time in the operating room because it’s totally customized to the patient.”
“We are meticulously and incrementally expanding the scope of the clinical service and adding value to the hospital from the department of radiology,” he says. “By listening to the needs and analyzing the market, we have added additional 3D-printing hardware, including material jetting. This opens up new clinical service line opportunities, for example to more easily generate 3D-printed parts in multiple colors so that each anatomic part can be color-coded.” Rybicki also hopes to hire two more engineers to meet the demand and support the more complex work of creating surgical guides. The sticking point is funding.
As an emerging technology, 3D printing is currently assigned a Category III CPT code. (Rybicki was a driving force behind this code, and now he serves on the ACR Economics Commission.) Under this category, reimbursement for 3D printing is lacking compared to the amount of work required to create 3D-printed models for patient care, Rybicki says.
To secure a universal Category I code, which offers higher reimbursement, extensive data is needed to demonstrate 3D printing’s widespread impact on patient care. But such data is limited because not every radiology practice can afford a 3D-printing lab and their inevitable growth. Moreover, data that shows value of clinical services often comes from clinical trials. “It’s kind of a chicken and egg situation,” Rybicki explains. “As soon as data accrues from more than 50 and preferably from 100+ medical centers, we’ll build the needed components for a Category I code. However, it’s hard to get these data because only bigger and more committed hospitals can afford 3D-printing labs, and funding for clinical trials requires resources and protected time for radiologists to lead.”
To capture the 3D-printing data that is available, Rybicki and Mahoney strongly support the 3D Printing Registry, a joint venture of the ACR and the Radiological Society of North America. The registry collects anonymized 3D-printing case information to better understand how 3D models are made, what images are used in their creation, and how they impact clinical care. They are also looking for ways to understand the cost savings that comes from 3D printing. “We need benchmarks for the cost savings to individual healthcare systems that 3D printing provides,” Mahoney says. “As these benchmarks are developed, we can translate 3D printing into dollars and cents saved, which will help build a stronger case for higher reimbursement.”
Although work still needs to be done to understand the return on investment of 3D printing, Mahoney is certain that the technology represents a game changer in patient care and a new frontier in radiology. “Radiologists have never shied away from technological advances. We’ve always been a group of physicians who’ve said, ‘Bring it on, and we’ll see how we can use it to improve patient care,’” she says. “3D printing brings so many opportunities for care improvement. I’m convinced that this is the way of the future.”
Hinna Danesi is one of only a dozen surgeons worldwide who perform endoscopic multi-valve heart surgery. Before joining the UC Medical Center in March of 2021, he had successfully conducted the procedure in cases involving one and two valves in his native Italy, but he knew that accessing three valves through one small incision would be difficult.
“Heart valve location varies among patients, and in the diseased heart it is even more unpredictable. You cannot access all four valves from one unique site on the chest without a thorough understanding of the patient’s anatomy,” Hinna Danesi explains. “The access point for the aortic valve, for instance, is different from the one for the mitral, tricuspid, and pulmonic valves.” Thanks to innovations in UC Medical Center’s radiology department, Hinna Danesi could approach the surgery more prepared than ever before.
Several years earlier, Frank J. Rybicki, MD, PhD, vice chair of imaging operations and quality in at UC Medical Center, established the department’s 3D-printing section. The clinical service uses CT and MR images to create personalized medicine via anatomic models, anatomic guides, and digital surgical planning. The anatomic models allow surgeons, like Hinna Danesi, to plan and even practice their procedures.
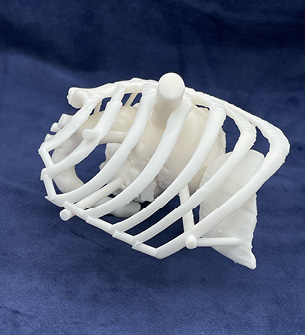 The 3D printing lab at the UC Medical Center uses advanced imaging to create anatomic models that surgeons and other providers use to plan procedures. |
Recruiting a 3D-printing Expert
Rybicki formed the 3D-printing lab after joining UC Medical Center in 2019. Mary C. Mahoney, MD, UC Medical Center’s chair of radiology, had a longstanding interest in 3D printing based on its proven impact on patient care and recruited Rybicki in part to establish the lab.“The more I thought about it, the more applications I saw for this technology. For instance, I envisioned patient-specific 3D-printed guides for more accurate placement of radiation seeds in patients with a post-surgical deformity,” Mahoney says. “I got excited about it, and the literature supported my instincts that radiology is becoming more patient-centric and 3D printing is the best way to carry that into the future for Cincinnati and as a profession.”
 Frank J. Rybicki, MD, PhD, UC Medical Center’s vice chair of imaging operations and quality in radiology, co-chair of the ACR 3D Printing Registry Governance Committee, and member of the ACR Economics Commission, established the 3D printing lab after joining the medical center in 2019. |
“I was well aware of Frankie’s work because it had received so much attention in the media and the radiology world, particularly his work on the face transplant. We had also known each other years before as we both worked on the ACR Committee on Appropriateness Criteria,” Mahoney says. “His name surfaced again when a former colleague of mine who co-launched the renowned 3D-printing section at the Mayo Clinic Rochester, Jane Masumoto, mentioned that Frankie might be able to launch and lead our program. I got in touch with him and that’s how it all began.”
Forming the Lab
Once at UC Medical Center, Rybicki relied on his leadership skills and experience establishing 3D printing as a clinical service line in Boston and Ottawa. Through her conversations during tumor boards, Mahoney had already ensured that the surgeons would use the models, so Rybicki focused on developing the lab itself. That required securing space to house the lab, acquiring dedicated software, purchasing a 3D printer, and building rapport with colleagues. Rybicki launched the lab with the help of a radiology resident and a cardiothoracic imaging fellow after building a dedicated computer from parts, obtaining a trial software license, and purchasing a desktop printer. “Besides an invested radiologist, these are the bare bones of what you need to start a 3D-printing lab,” Rybicki says.In outfitting the lab, Rybicki considered two types of desktop printers, each of which uses a different printing method. One is called vat polymerization and the second is called material extrusion. Vat polymerization printers use ultraviolet light that converts a vat of polymer resin into a physical 3D-printed model. Material extrusion printers share similarities with glue guns; they dispense one or more heated polymers through a printer head and onto a build plate, depositing each successive two-dimensional layer to create the 3D-printed part. “Schools and universities commonly use these two types of printers,” Rybicki explains.
Rybicki initially setup the printing lab in a vacant room within the radiology department. But he and the trainees were inundated with requests for models, and the group needed more room for a second printer and space with good ventilation to control the strong fumes that 3D printing produces. Recognizing the growth in the clinical service, Mahoney saw an opportunity to move the lab into a new space that was created as part of an already planned departmental renovation project. The new space includes a negative air pressure system, space for sterile operations, and proper desktops and water facilities for a mid-sized 3D-printing lab within a medical center.
Printing a Model
In addition to moving the lab to a larger, better equipped space, Rybicki expanded his small team to include an engineer with experience operating and maintaining 3D-printing equipment to meet the growing clinical demand. As the demand grew even further, Rybicki recruited a second engineer who had worked in the 3D-printing lab at Walter Reed National Military Medical Center. “As the lab expanded to include cutting guides, craniomaxillofacial reconstructions, and dental applications, it was clear that we needed to recruit someone with extensive experience in metal printing, in particular, so that we can expand our portfolio of clinical services in the future,” Rybicki says. Mary C. Mahoney, MD, UC Medical Center’s chair of radiology, recognized the potential of 3D printing to significantly improve patient care. She recruited Rybicki in part to establish the department’s 3D printing service line. |
With the help of an engineer, Rybicki will then segment the patient’s MRI or CT images to create a digital blueprint of the model. He also transfers the imaging information from the digital imaging and communications in medicine file format to a stereolithography file format. “Printing a model includes translating the imaging data from radiology language into manufacturing language so that the 3D printer can recognize it,” Rybicki explains. “Then we send that information to the printer to create the model, a process that can take between six to as many as 30 hours.”
Given the time and cost associated with printing a model, the team makes them for only complex cases. Once a model is completed, Rybicki meets with the surgeon again to review the model. From there, the surgeon can use the model to better understand the anatomy before entering the operating room. The surgeon will often practice on it. “They might drill or cut through the model as they’re deciding how to access a brain tumor, for example,” Rybicki explains. “Occasionally, the surgeon will sterilize the model and take it into the operating room as reference. It’s a game changer for surgeons, and they continue to ask for it.”
Customizing Care
In the triple valve case, Hinna Danesi used the model to determine where he should make the incision that he needed to repair the patient’s heart. “The 3D modeling allowed me to see exactly where the patient’s valves were located and also the relation among them so that I could plan the best access to operate on all of them,” Hinna Danesi explains. “Dr. Rybicki made me feel like a sniper, targeting the valves and allowing me to keep the incision to less than 1 inch. Although I could have performed the surgery without the 3D model, I can assure you that having a prepared idea of the anatomical relations of the specific patient’s valves, especially in a 3D-computed model, is something priceless that I will not waive for any patient undergoing endoscopic surgery from now on.”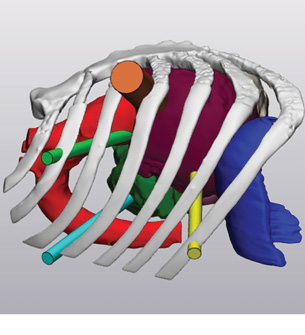 Printing a model involves segmenting the patient’s images to create a digital blueprint of the model. |
While the lab started out creating models for surgical planning, Rybicki and his team recently expanded its scope. The clinical service now creates personalized surgical guides for craniomaxillofacial reconstruction. For example, if a patient loses part of their jaw from a tumor or trauma, the team can use imaging to map the exact shape of the void. From there, they can 3D print a guide that the surgeon can use to more precisely reconstruct that part of the bone and the necessary blood supply for a successful procedure. “The guides are like cookie cutters that the surgeons can use to cut the bone, and it will be the perfect size and shape with all of the blood vessels intact,” Rybicki says. “It significantly reduces the amount of time in the operating room because it’s totally customized to the patient.”
 Cardiovascular surgeon Tommaso Hinna Danesi, MD, used a 3D printed model to help him determine where to make the incision in the nation’s first triple-valve surgery. |
Illustrating the Impact
Since UC Medical Center’s 3D-printing lab opened in 2019, demand for the models has increased from roughly 80 over the first year to several per week. As the number of orders has risen, Rybicki has added four additional printers to the lab.“We are meticulously and incrementally expanding the scope of the clinical service and adding value to the hospital from the department of radiology,” he says. “By listening to the needs and analyzing the market, we have added additional 3D-printing hardware, including material jetting. This opens up new clinical service line opportunities, for example to more easily generate 3D-printed parts in multiple colors so that each anatomic part can be color-coded.” Rybicki also hopes to hire two more engineers to meet the demand and support the more complex work of creating surgical guides. The sticking point is funding.
As an emerging technology, 3D printing is currently assigned a Category III CPT code. (Rybicki was a driving force behind this code, and now he serves on the ACR Economics Commission.) Under this category, reimbursement for 3D printing is lacking compared to the amount of work required to create 3D-printed models for patient care, Rybicki says.
To secure a universal Category I code, which offers higher reimbursement, extensive data is needed to demonstrate 3D printing’s widespread impact on patient care. But such data is limited because not every radiology practice can afford a 3D-printing lab and their inevitable growth. Moreover, data that shows value of clinical services often comes from clinical trials. “It’s kind of a chicken and egg situation,” Rybicki explains. “As soon as data accrues from more than 50 and preferably from 100+ medical centers, we’ll build the needed components for a Category I code. However, it’s hard to get these data because only bigger and more committed hospitals can afford 3D-printing labs, and funding for clinical trials requires resources and protected time for radiologists to lead.”
To capture the 3D-printing data that is available, Rybicki and Mahoney strongly support the 3D Printing Registry, a joint venture of the ACR and the Radiological Society of North America. The registry collects anonymized 3D-printing case information to better understand how 3D models are made, what images are used in their creation, and how they impact clinical care. They are also looking for ways to understand the cost savings that comes from 3D printing. “We need benchmarks for the cost savings to individual healthcare systems that 3D printing provides,” Mahoney says. “As these benchmarks are developed, we can translate 3D printing into dollars and cents saved, which will help build a stronger case for higher reimbursement.”
Although work still needs to be done to understand the return on investment of 3D printing, Mahoney is certain that the technology represents a game changer in patient care and a new frontier in radiology. “Radiologists have never shied away from technological advances. We’ve always been a group of physicians who’ve said, ‘Bring it on, and we’ll see how we can use it to improve patient care,’” she says. “3D printing brings so many opportunities for care improvement. I’m convinced that this is the way of the future.”
Creative Commons
Creating 3D Models from Imaging is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License . Based on a work at www.acr.org/imaging3. Permissions beyond the scope of this license may be available at www.acr.org/Legal.Share Your Story
Have a case study idea you’d like to share with the radiology community? To submit your idea, please click here.Now It’s Your Turn
Follow these steps to begin establishing a 3D printing lab in your department. Tell us how you did at imaging3@acr.org or on Twitter with the hashtag #Imaging3 .
- Appoint or hire someone who is passionate about 3D printing to build out the lab, including purchasing a printer, a dedicated computer and software, finding adequate space, and eventually hiring engineers to round out a clinical service.
- Socialize the clinical service to other hospital leaders and help them understand that despite the costs, 3D printing adds value to patient care and is an indispensable asset to the healthcare facility.
- Contribute to the 3D Printing Registry to help improve patient care and build a case for greater reimbursement.
Author
Jenny Jones, Imaging 3.0 managing editor
Join the Discussion

Want to join the discussion about how radiologists
can lead quality improvement projects for improved
image ordering? Let us know your thoughts on
Twitter at #imaging3.
#Imaging3 on Twitter
Call for Case Studies
