Radiologists agree on the importance of breast cancer screening and are taking steps to improve access and empower women to make informed decisions. Click here to see steps you can take in your community and practice.
With a 25-year career that has involved toppling silos, breaking glass ceilings, and leading changes that have improved mammography screening access for millions of women, Dana H. Smetherman, MD, MPH, MBA, FACR, is setting the pace for the future of her profession. Although she never intended to be an industry pioneer when she entered the medical field, her problem-solving personality and insatiable curiosity have pushed her to reimagine the ways that she can add value as a radiologist.
“Throughout my career, I’ve had opportunities to be a changemaker because I’m always open to trying a different approach,” says Smetherman, chair of the radiology department at Ochsner Medical Center and secretary-treasurer of the ACR. “My husband kindly calls me ‘intellectually curious,’ but I think it’s more of a restlessness, a desire to keep learning new things and finding better solutions. I’m always asking, ‘How can we do this better or make this easier for everyone?’”

Dana H. Smetherman, MD, MPH, MBA, FACR, is passionate moving imaging forward to increase the value that radiologists bring to patient care.
|
Smetherman’s restless spirit has led her to the top of nearly every organization she’s joined throughout her professional career, both in New Orleans and at a national level. By working across departments to reinvent the patient experience, Smetherman is pioneering a new path for radiology.
Searching for Purpose
Smetherman grew up in New Orleans, the oldest of four daughters born to her father, a lawyer, and her mother, a dance teacher. Her interest in medicine developed around age 10 when she watched her best friend’s father, a physician, examine her younger sister when she had pneumonia. “I remember watching him work and thinking, ‘I can see myself doing this instead of the jobs I see my parents doing,’” Smetherman says.
While she flexed her creative muscles in choir, plays, and musicals and spent summers working at her uncle’s law firm during high school and college, Smetherman remained committed to her interest in medicine. To explore this interest further, Smetherman volunteered at the local hospital during her senior year of high school, serving as an assistant in the operating room. “That really solidified my career path,” she says. “I knew I wanted to pursue healthcare because it gave me a sense of purpose to provide a fundamental service to make people’s lives better.”
Smetherman ended up following in the footsteps of her great-grandfather, her only relative known to have worked in medicine. Through the generations, her family passed down stories about him, a small-town doctor who earned his medical degree at Tulane University in 1908 and died just 10 years later during the 1918 flu pandemic after contracting the illness from a patient. Smetherman prizes his possessions — including his old medical license, diploma, and microscope — as reminders of the legacy she carried into the medical profession.
However, to make the long-lasting impact she wanted to have as a physician, Smetherman realized she would have to let go of legacy thinking and pioneer new ways to improve care.
Exploring Public Health
After graduating from Harvard with a degree in biology, Smetherman returned to New Orleans for medical school at her great-grandfather’s alma mater, Tulane University. She was drawn to Tulane’s combined MD/MPH degree program, which allowed her to simultaneously earn a medical degree and a public health degree in just four years for the cost of a single degree.

Smetherman (right) pictured with medical school classmates Angela T. Barthe, MD, and Christoper A. Hinnant, MD. |
Although she didn’t realize it at the time, these combined studies would end up serving her well throughout her career. “I’d love to say that I had this beautiful line of sight that I was going to wind up in breast imaging, which is one of the fields where population health is really important for screening,” Smetherman says. “But I can’t say that I had that much foresight. It just seemed like a good financial value and an interesting opportunity for someone who loved school as much as I did.”
The program offered electives that counted toward both degrees. For one of those electives, Smetherman participated in a three-month rotation in Belize where she encountered medical care and public health issues in remote villages. “It was eye-opening to see the difference between a place like Belize and the U.S.,” she says, recalling the lack of medical equipment, basic antibiotics, and, in some areas, even plumbing. “It gave me a much deeper appreciation for the health challenges facing different populations.”
The experience shifted Smetherman’s perspective, preparing her to consider the diverse issues that patients face and shaping the way she approaches care to this day.
Discovering the Right Specialty
After finishing medical school, Smetherman completed her internship at Ochsner Medical Center in New Orleans. From there, she decided to pursue a specialty in neurology hoping that it would position her to have an immediate impact on patient care. But soon after entering a residency program at Yale University, she realized that the field wouldn’t allow her to impact day-to-day patient care the way she had envisioned.
“I really enjoyed the hospital environment: figuring out what was wrong with patients and seeing them improve with treatment,” she says. “But until I started my residency, I didn’t fully appreciate that these physicians spent most of their time in the clinic, managing people with chronic diseases over time. I felt powerless to help people or fix things that were out of my control, like whether patients had insurance or transportation to therapy. I knew it wasn’t the right fit for my personality because I wanted to be able to see that I was making a difference.”
Halfway through the residency program, Smetherman stepped back to reassess her options and find a specialty in which she could directly impact patient outcomes every day. Having worked closely with neuroradiologists and neuropathologists during her neurology residency, Smetherman called former classmates who pursued those specialties, asking why they chose each discipline and how they spent their days.
“From those conversations, I realized that radiology would give me the chance to impact a lot of different patients,” Smetherman says. “It was about solving puzzles to diagnose patients, which was what had drawn me to neurology in the first place. But having the ability to use imaging to look inside someone to answer those questions — that’s what really sealed the deal.”
One of her medical school classmates and fellow interns told her about an opening in Ochsner’s radiology residency, and she interviewed for the program while home on Christmas break. Once accepted to the program, Smetherman entered every radiology rotation with an open mind and eventually found her niche in breast imaging, where she saw emerging screening technologies as opportunities to innovate and advance patient care.
“Breast imaging turned out to be the perfect fit for my personality,” she says, “because you’re involved in every step of the patient’s journey — from screening and diagnosis to biopsy and treatment — so you can see a nearly real-time impact throughout every stage of care. I found that fulfilling, and with screening mammography just starting to take off, it was the perfect time to pursue breast imaging.”
Learning to Lead
Smetherman entered her first leadership role in radiology when she was appointed chief resident during her final year. “Even as a young resident, Dana demonstrated maturity and fairness. She did an admirable job managing the interests of her co-residents,” says Edward I. Bluth, MD, who was chair of the radiology department at that time. “She showed all of the qualities and traits of a natural leader by carefully considering the subtleties of every situation before making a decision.”

Smetherman was promoted to chair of Oschner’s radiology department in 2019. At the same time, she became the hospital’s first female associate medical director. |
With the responsibility for managing call schedules for radiology residents as well as for developing moonlighting schedules in the emergency department, Smetherman discovered the delicacy of juggling multiple interests and successfully managing people. “Dana pays great attention to detail and understands issues at a granular level,” says James M. Milburn, MD, vice chair of academic affairs for the department of radiology, residency program director, and leader of the interventional neuroradiology section, who was an intern and resident alongside Smetherman at Ochsner. “Her supervisors have continually promoted her throughout her career because she’s extremely reliable and well respected throughout the medical community.”
Ochsner’s collegial culture drew Smetherman to join its staff in 1996. Enamored with the hospital’s multispecialty practice, she encountered many opportunities to collaborate with diverse teams focused on a common goal of optimal care. She also had the chance to work with mentors, including Gunnar J. Cederbom, MD, Ochsner’s section head of breast imaging at the time.
A model for multidisciplinary collaboration, Cederbom partnered with other departments to introduce new imaging innovations, like the region’s first stereotactic biopsy unit, which Ochsner opened at the beginning of Smetherman’s residency. “Dr. Cederbom worked closely with breast surgeons, medical and radiation oncologists, pathologists, and other members of the multidisciplinary team to help introduce image-guided needle biopsies, brachytherapy, and wire localizations before a lot of hospitals were doing those kinds of things,” Smetherman says. “We’ve always been focused on working as a team to coordinate better care for our patients.”
Streamlining the Patient Experience
In 2001, as Cederbom began to reduce his clinical time at Ochsner, Bluth promoted Smetherman to section head of breast imaging. “I knew she had the focus and dedication to lead the department forward,” Bluth says. “She wasn’t satisfied with the status quo; she wanted to see things continually improve.”
Smetherman stepped into the role just after Ochsner’s breast imaging section moved into a free-standing multidisciplinary breast center. She embraced the change and saw the new location as a chance to redesign the entire patient journey. In typical fashion, she got right to work.
Recognizing that patients were often waiting more than a week for abnormal mammography results and then enduring a drawn-out process for follow-up imaging and biopsies, Smetherman developed an ecosystem of multidisciplinary breast specialists who work in coordination to streamline the patient journey. She hired a nurse navigator to immediately call patients with abnormal results, arrange radiologist/patient consultations, coordinate additional exams and image-guided biopsies, and schedule appointments for surgery, if needed.
The approach has reduced the time between abnormal mammograms and biopsies from more than a week to one or two days, dramatically alleviating anxiety for patients awaiting their results. “Some patients say that the time between an abnormal screening, a biopsy, and a diagnosis is the most stressful time in their entire lives,” Smetherman says. “By taking ownership of the process, we can guide patients quickly and smoothly through the continuum of care. It’s been gratifying to make the process more seamless and less stressful for patients. Ensuring fewer sleepless nights for them is so fulfilling for me.”
Leading Through Disaster
Smetherman’s take-ownership approach also served her well when Hurricane Katrina struck New Orleans in 2005. Smetherman happened to be on call the weekend that the storm hit and was expected to report to the hospital with two other radiologists. “One of my colleagues called and asked if I wanted to switch shifts so that I could evacuate with my family, but my kids had al-ready left with my sister,” she says. “So I said, ‘Nope, I’m committed to stay.’”

Smetherman (fourth from left) was part of “Team A,” which helped keep Oschner operating during Hurricane Ida. The hurricane made landfall as a Category 4 on Aug. 29, 2021, 16 years to the day after Hurricane Katrina. |
At the time, Smetherman didn’t imagine that she would be stuck at the hospital for nearly a week. Hurricane Katrina made landfall as a Category 3 storm — devastating New Orleans with winds and rains that wiped out roads and knocked out power. “After the storm, I remember going up to the hospital’s roof and seeing that the roof of the Superdome was ripped off. There were trees down and debris everywhere,” she says. “But it wasn’t until the next day, when the levees started breaking, that the damage became catastrophic.” The surge engulfed homes along the bayou, displacing hundreds of thousands of residents.
To keep the radiology department functioning throughout the disaster, Smetherman displayed agility — both in her leader-ship and in her ability to literally run around the hospital, processing imaging exams with limited access to electricity or equipment. “We got down to one generator for the whole facility, which didn’t leave our department with a whole lot of power,” she says. “We had to stage the portable units on the intensive care unit (ICU) floors, carry the imaging plates upstairs to take the radiographs, then bring them back downstairs to process them.”
As a result of the team’s preparation and dedication, Ochsner was the only full-service hospital in the area to continue accepting patients throughout the disaster. And Smetherman made sure the public knew that the hospital was open for them. “There was no communication with the outside,” Milburn says. “So, to show the helicopters flying overhead that our hospital was open, she came up with a plan to put a huge sign on top of our parking garage using red trash bags to spell OPEN. She was right there on the front lines, even in a scary situation, looking for innovative solutions to help our patients.”
(Hurricane Ida hit New Orleans just as this publication was headed to press. Once again, Smetherman was on the front lines, providing care during one of the strongest storms to ever hit the city.)
Embedding Value
Ochsner’s ability to care for patients even while the city was under extreme duress during Katrina bolstered its reputation. As a result, the hospital, which before had been a multispecialty practice that primarily provided tertiary care, began a rapid growth trajectory of acquiring other hospitals and primary care centers across the region. “We in radiology expanded from being specialists to becoming stewards of care for the whole community,” Smetherman says. “All of a sudden, we had the chance to screen more patients, which presented more opportunities to make that process easier and more accessible.”
This growth marked a turning point in Smetherman’s perspective as a radiologist. Instead of focusing solely on individual patients, she began leveraging her public health background to reimagine how services were delivered to the entire population. She focused on reducing screening wait times, which increased as Ochsner’s mammography volume grew, leaving some women to wait a month for screening mammography. “As I was hearing the same pain point from several different people,” Smetherman says, “I started thinking about what we could do differently to solve the problem.”
Smetherman partnered with Pedro Cazabon, MD, then chair of Ochsner’s primary care department, where many complaints about access to mammography screening originated. Together, they conceived the idea to embed a mammography unit within the primary care office, offering same-day screening access to patients who were visiting their primary care physicians. “The patients loved it because they didn’t need to schedule an appointment; they could just walk down the hall,” she says. “The internal medicine doctors loved it because we were able to work together to take care of these patients. That’s when I realized that we could really make a difference in population health by working together.”
The embedded mammography pilot program was so successful that it became a blueprint for other primary care units across the health system. Now, when Ochsner builds new outpatient clinics, mammography units are incorporated from the outset. “It was the beginning of a great collaboration between breast imaging and primary care with the patient at the center,” Smetherman says. “It was so gratifying to work with those colleagues to make screening easy and accessible. It showed me how radiology could add value for our patient population.”
Expanding Screening Access
By then, Smetherman’s influence was already extending beyond Ochsner. Shortly after joining the hospital in 1996, Smetherman accepted Bluth’s invitation to join the Radiological Society of Louisiana, the state chapter of the ACR. At her first meeting, Smetherman looked around the room and realized that she was the only young woman in attendance.

Smetherman has been an active ACR member for many years. This photo is from ACR's 2017 Annual Meeting. |
Rather than feel intimidated, Smetherman got more involved, eager to introduce different viewpoints into the conversation. Eventually, she was elected as the chapter’s secretary-treasurer before rising to the role of vice president, then president, and, finally, councilor. “I’m so grateful that Dr. Bluth nominated me to take on leadership roles, both within the department and the state chapter,” Smetherman says. “Being involved at that level gave me a broader purview of the radiology profession, which showed me the additional value you could bring to your practice by knowing what was happening outside of your own organization.”
In 2011, Smetherman’s involvement in the radiology profession expanded more when Ochsner hosted a meeting for radiologists from multispecialty practices nationwide — including Geraldine B. McGinty, MD, MBA, FACR, then chair of the ACR Commission on Economics. After hearing Smetherman’s presentation about the value of embedding screening mammography into primary care clinics, McGinty encouraged her to take on a larger role within the ACR.
Smetherman collaborated with McGinty on a few projects before joining the Commission on Economics and the Commission on Breast Imaging, which, at the time, were both working to expand coverage for digital breast tomosynthesis. “Being on the breast commission with the luminaries in our field who have led the way on standardized reporting and screening recommendations was an incredible honor,” Smetherman says. “And simultaneously working with the economics commission gave me the opportunity and privilege to impact patient care for hundreds of thousands of women in ways I never imagined when I decided to become a radiologist.”
When the ACR introduced its Breast Screening Leadership Group, an extensive training course for future screening leaders, McGinty invited Smetherman to join the inaugural class of 2015. “That experience gave me a different perspective on screening access as I started to think about helping patients beyond New Orleans,” says Smetherman, who has continued to increase her involvement with the ACR, serving as vice chair and then chair of the Commission on Breast Imaging’s Economics Committee before rising to vice chair and then chair of the commission itself. As commission chair, Smetherman also joined the ACR Board of Chancellors, becoming secretary-treasurer in 2021. “The ACR has given me the chance to help address disparities in care, not just on a one-to-one basis, but on a larger scale by making screening more accessible.”
Setting a Strong Example
While deepening her involvement nationally, Smetherman also expanded her hospital leadership role, joining the Ochsner Health Foundation Board in 2013 and becoming its first woman physician member. “I never set out to be a pioneer, but sometimes you don’t realize you’re setting an example until you look around the room and notice that you’re the only woman there,” says Smetherman, who’s glad to see several more female physicians on the board now. “I was fortunate to have mentors, like Dr. McGinty, giving me opportunities and encouragement along the way, and if I had any impact on other women’s decisions to pursue leadership roles in this profession, then I’m quite proud of that.”
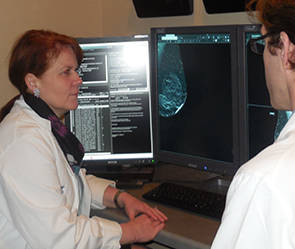
Smetherman found her calling in breast imaging, which allows her to have a direct impact on patient care. |
This wasn’t the first or last time that Smetherman broke the glass ceiling. She was the first female officer, president, and councilor in her state chapter. Then in 2019, at the same time she became the first female chair of the radiology department at Ochsner Medical Center, Smetherman also became the hospital’s first female associate medical director over specialties such as emergency medicine, infectious diseases, gastroenterology, endocrinology, and rheumatology — a rare role for a radiologist.
“The associate medical director position intrigued me even more than the role as radiology chair because it gave me a chance to see so much more of the patient’s whole experience,” says Smetherman, who regularly rounds in the departments she oversees. “Some people might think it’s odd to have those departments reporting to a radiologist, but radiology is uniquely positioned to be the convener because we interact with almost every specialty, and we touch a lot of patients in their journey. That collaboration enables better care coordination, which makes the whole institution stronger.”
Smetherman’s experience on numerous committees at Ochsner also makes her well-suited for the associate medical director role. She has served on and chaired the hospital’s medical advisory committee, compensation committee, and executive committee on continuing medical education. “Dana has collected a tremendous amount of insight and knowledge throughout her career, and because of that, people respect her as a leader — not just in our organization but throughout the industry,” says Warner L. Thomas, president and CEO of Ochsner. “She’s always tasked as a leader when we start big projects because she’s willing to challenge the status quo and do things differently to raise the quality of care.”
Gaining Business Insight
Through her involvement in both the Ochsner board and the ACR, Smetherman developed a deeper interest in the business side of medicine. To further her business acumen, she decided to pursue her Master of Business Administration (MBA) in 2015, at age 52. She entered an online MBA program, which gave her the flexibility to balance her professional schedule and the rigorous course load. “I timed it when my children were starting high school, so we were all studying and writing papers together in the evenings,” says Smetherman, whose twin son and daughter recently turned 20. “It was a lot of late nights, early mornings, and long weekends. It wasn’t easy, but I’ve always loved learning new things.”
With a concentration in entrepreneurship, Smetherman’s degree covered economic theory, organizational behavior, change management, and other business-centric topics that proved valuable in her leadership roles — especially as radiology began shifting toward a value-based care model. “Being a constant learner is part of what makes Dana great at what she does,” Thomas says. “She’s always looking for new knowledge and better solutions, and that’s what makes her a changemaker and trailblazer.”
Besides the business topics she expected to learn, Smetherman was surprised to gain a crash course in virtual learning. “It gave me a better appreciation for what education is like now and how to use tools like screen sharing and virtual meetings to collaborate remotely,” says Smetherman, who earned her degree in 2017. “Those weren’t originally the skills I thought I would acquire with my MBA, but they turned out to be quite valuable as time went on.”
Rethinking Remote Radiology
Smetherman soon learned to rely heavily on remote collaboration tools when COVID-19 flared in New Orleans in 2020. Pulling from her disaster management experience with Hurricane Katrina, she promptly developed an emergency plan to keep her team operating throughout the pandemic. “We immediately implemented social distancing protocols to limit contact between radiologists, technologists, residents, and medical students in our department,” Smetherman says. “We’ve always had people packed together in the reading rooms because we want trainees to be near the attending physicians. To maintain that same collaboration without the physical closeness, we had to get creative.”
Ochsner quickly escalated its previous plans to deploy remote workstations, allowing radiologists to work from home when COVID-19 cases spiked in March of 2020. (Read more about the department’s COVID-19 response in
this Imaging 3.0 case study) “With more people working remotely to lessen the density of people in the reading rooms, we started using digital communication tools more and more, especially the real-time chat feature in our picture archiving and communications system,” Smetherman explains. “Once we figured out how to function without all our radiologists sitting inside the hospital, we were able to transition our whole emergency radiology section to remote work.”
This work-from-home flexibility has brought unexpected benefits. Now, Smetherman is beginning to recruit new radiologists who can contribute to the team remotely — an approach that she expects will strengthen the department’s subspecialty bench, which has traditionally been difficult to fill. “We were limiting ourselves before by not even considering recruits who couldn’t re-locate here, and the pandemic forced us to reimagine a nimbler approach,” Smetherman explains. “We never would have been this open-minded if we had just stuck with our legacy thinking and assumed that radiologists had to be in the hospital to add value.”
Refreshing Her Focus
It’s this pioneering attitude that sets Smetherman apart. Even with a busy clinical schedule and multiple leadership roles within the hospital, the ACR, and the broader industry, she remains committed to blazing paths to move the profession forward.

When she’s not working, Smetherman enjoys traveling with her husband, Charles Freeman, and their twins. |
To manage the stress of it all without losing her spark, Smetherman recharges and revitalizes with family time and travel. She and her husband, Charles Freeman, have traveled around the world with their twins — including trips to Greece, Spain, Italy, Scotland, Jamaica, and Peru — and throughout the U.S. and other parts of North America.
But even when she can’t travel far, Smetherman prioritizes time to unplug. About five years ago, she and her husband built a small beach house about an hour from New Orleans. “We try to go there on the weekends that I’m not working, but it’s close enough that we can go for the day,” she says. “Just being in a different place and walking on the beach helps me clear my head and come up with new ideas. Being outdoors has been very important, particularly during this stressful time, and especially as a radiologist who might not even look out of a window all day.”
With an enduring artistic spirit, Smetherman also relies on music to help her unwind. Although she mainly sings in the seclusion of her car these days, Smetherman used to share her musical and acting talents with patients and colleagues. During medical school, she was part of a theater troupe that performed monthly plays in the pediatric ward and produced larger shows annually. Around the same time, she briefly filled in as the lead singer of a rock band. Now that her children are both in college, Smetherman is considering picking up her musical pursuits again. “I’m still friends with my voice teacher, so hope springs eternal,” she says.
Whether she’s traveling with her family, enjoying the outdoors, or singing along with her favorite songs, Smetherman relishes her downtime. It gives her the headspace to continue reimagining radiology as healthcare evolves. “I’m focused on looking at the horizon and building for the future beyond COVID-19,” she says. “With all the challenges of the pandemic, we need something to be optimistic about, and there are so many exciting opportunities right now to grow our department and add value through radiology.”
At age 57, Smetherman has no intention of slowing down or even considering retirement as she looks to continue improving care through innovative initiatives and multidisciplinary collaboration at Ochsner. “It’s so exciting and gratifying to be part of a bigger vision to make a difference in the Gulf South and impact the health and wellness of our whole state,” she says. “As my career has progressed over 25 years, I’ve had opportunities to become a changemaker that have enabled me to feel like I’m making a much larger difference beyond just taking care of each patient. Yet, there’s so much left to do. I feel like I’m just getting started.”








