As a child, Arun Krishnaraj dreamed of being a sports prodigy. Growing up near the University of North Carolina at Chapel Hill (UNC) in the 1980s, he aspired to join a team of Tar Heels stars like Michael Jordan and eventually replace the program’s legendary head coach, Dean Smith.
Unfortunately, given his relatively modest height and speed, Krishnaraj had to accept the reality of his athletic potential. “When I hit my maximum height of five feet nine inches, I knew that my trajectory in basketball was limited,” he jokes. “If I was six inches taller, maybe I wouldn’t have studied as hard in school.”

Arun Krishnaraj, MD, MPH, FSAR, has a strong vision for the future of radiology. |
Instead, Krishnaraj followed his family’s lead and pursued a career in medicine. He ultimately selected a specialty in academic radiology because it afforded him the opportunity to combine his innate teaching abilities, tech savviness, and innovative spirit to coach a different kind of team.
Now, as chief of the body imaging division at the University of Virginia (UVA) Health System, Krishnaraj is prioritizing curiosity and care to pave a path for the future of radiology. By embodying the values of patient- and family-centered care, Krishnaraj models the vital role that radiologists can play — even as imaging technology evolves.
“I’m committed to addressing the frustrations that patients encounter throughout their healthcare journey and advocating on their behalf,” Krishnaraj says. “My mission is to figure out how we can take all of this great emerging technology to make imaging more accurate, accessible, and understandable so that it empowers patients to participate in shared decision-making.”
Family Tradition
Krishnaraj comes by this drive naturally. His father, Muthaiya Pillai Krishnaraj, known as Raj, was a pioneer as the first in his family to pursue a medical career and, eventually, the first to immigrate to the U.S. from southeastern India. As a general practitioner in a rural clinic outside of Pondicherry (now known as Puducherry), India, Raj often received chickens or other non-monetary goods as payment for medical services.
When another family member urged him to pursue the American dream, Raj reluctantly agreed to take an international licensing exam — letting his decision about whether to move to the U.S. ride on the outcome of his score. When he passed by a single point, it sealed the family’s fate. He flew to the U.S. to begin a psychiatry residency, and his wife and oldest son subsequently joined him in Philadelphia, where Krishnaraj was later born.
By the time Raj completed his medical training, the family was ready to escape Philly’s snowy winters for a warmer climate. He found an opportunity at a state psychiatric hospital in Goldsboro, North Carolina, where he ended up spending his entire 40-year career and raising his family. His older son followed his footsteps into medicine and became an internist who still practices in North Carolina.
For Krishnaraj, the decision to pursue a healthcare career wasn’t an easy one — in fact, he initially rebelled against it. “As an Indian immigrant, there’s both a stereotype and a cultural pressure to pursue a career in medicine,” he says. “It’s not that I didn’t respect what my father and brother did, I just wanted to do my own thing. I hated being pigeonholed just because I am of Indian descent.”
Study Abroad
As a student, Krishnaraj loved learning about a variety of subjects, from sports to space travel. “I was like a sponge, trying to learn as much about the world as possible,” he says. “As a digital native coming of age during the birth of the internet, I quickly learned how to use emerging consumer technologies to learn even more about the world.”
Recognizing his stellar academic performance and insatiable curiosity, Krishnaraj’s high school nominated him to participate in the North Carolina Governor’s School, a six-week residential summer program for gifted students. Living on campus at Salem College, Krishnaraj got to interact with other bright kids from across the state while taking classes focused on science. He graduated high school as valedictorian with SAT scores in the 99th percentile.
When the time came to make his college decision, Krishnaraj’s UNC fandom won out. He was accepted into the UNC honors program where advanced classes allowed him to explore various disciplines. Choosing UNC turned out to be a wise move not just academically but also personally. Krishnaraj ended up in a dormitory next to a young woman named Sarah, who had been one of his Governor’s School classmates and who eventually became his wife.
While considering study abroad at UNC, Krishnaraj found an opportunity in London that piqued his interest — more for the location than the specific field of study, which happened to be public health. “I worked for the National Health Service, shadowing the director of public health in a small district outside of London,” Krishnaraj says. “I was impressed with public health officers’ ability to budget healthcare equitably for the entire population in a nationalized health system. It was a striking difference from the healthcare system in the United States.”
After that summer abroad, Krishnaraj enrolled in the public health program at UNC. During his undergraduate studies, he worked with an epidemiologist named Bonnie C. Yankaskas, PhD, who was involved in the Breast Cancer Surveillance Consortium, a network of breast imaging registries conducting research to improve the delivery and quality of breast cancer screening across the U.S. Through this research and Yankaskas’ mentorship, Krishnaraj discovered that radiology combined his love of technology and his passion for public health.
“I knew radiology was the right specialty for me because I liked the diagnostic approach of gathering information to determine an answer using technology. You’re a bit of a detective in radiology, and that always appealed to me,” he says. “I realized that imaging and public health were a potentially powerful combination as screening technologies advanced.”
To explore this intersection of interests, he enrolled in a graduate program at UNC that allowed him to simultaneously earn a doctorate of medicine and a master’s of public health.
ACR Connections
Krishnaraj remained at UNC for his radiology residency, honing his leadership skills as co-chief resident of his class. “My role as chief resident was to advocate for the academic well-being of the residents,” he explains. “I loved the collaborative nature of facilitating education and cultivating interaction among medical students and physicians. It solidified my interest in academic medicine.”

Krishnaraj completed a two-year joint fellowship in informatics and abdominal imaging at MGH. Here, he stands in the famous Ether Dome, a historic amphitheater that was the site of the first public demonstration of ether as an anesthetic. |
It was also during residency that Krishnaraj began exploring leadership opportunities through the ACR. His residency program director, Paul L. Molina, MD, FACR, was president of the North Carolina Radiological Society, the state chapter of the ACR. Molina encouraged Krishnaraj to attend state chapter dinners and, ultimately, a national meeting of the ACR’s Resident and Fellow Section (RFS), which inspired Krishnaraj to run for a position on the RFS committee.
“I was impressed with the panel of RFS leaders at the time because they demonstrated that, even at a training level, you can have a prominent voice in an organization that advocates for patients,” Krishnaraj says. “My involvement in the ACR kept growing from there, and by the time I was a senior resident, I was voted chair of the RFS.”
At a national RFS meeting, Krishnaraj met James H. Thrall, MD, then chair of the radiology department at Massachusetts General Hospital (MGH) and chair of the ACR Board of Chancellors (BOC). Krishnaraj mentioned his interest in pursuing a fellowship at MGH, then one of the few departments offering specialized training in the emerging field of imaging informatics, which leveraged data-rich information technology to streamline radiology workflows and improve patient care.
While studying informatics, Krishnaraj wanted to simultaneously advance his clinical studies through an abdominal imaging fellowship. Thrall helped him arrange interviews with both the MGH informatics and the abdominal radiology faculty to facilitate an unusual two-year joint fellowship. Both departments instantly saw value in Krishnaraj’s desire to combine the two disciplines.
“I’ve interviewed scores of fellow candidates, and Arun stood out from the very beginning,” says Peter R. Mueller, MD, division head of abdominal imaging and interventional radiology at MGH, who’s retiring in 2022 after a 49-year medical career. “Within 30 seconds, I knew that I wanted to hire him as a fellow because he wanted to enhance the field and be involved in the future of radiology.”
In 2010, Krishnaraj, Sarah, and their newborn son, Nayan, moved from North Carolina to Boston for the fellowship opportunity. “For me, it was a great honor to train at one of the world’s most prestigious institutions,” Krishnaraj says. “I credit my early career arc to the people there.”
Fellow to Faculty
During his informatics fellowship, Krishnaraj worked closely with Michael E. Zalis, MD, an interventional radiologist and director of CT colonography. At the time, Zalis was developing one of the first electronic health record search engines. Krishnaraj’s job was to write clinical queries for the program to retrieve data buried in patients’ medical charts.
Krishnaraj devoted a couple of days a week to informatics projects like this and spent the rest of his time in the abdominal imaging fellowship. Even as a fellow, Krishnaraj demonstrated the characteristics of a charismatic leader.
“The diagnostic imaging area is typically dark and quiet, and radiologists have their heads down reading images,” Mueller explains. “But when Arun was here, he wasn’t just reading CTs. He was always happy and smiling and talking to other staff. He sincerely related to everyone around him; it wasn’t just the doctors and the referring physicians, it was the technologists, the nurses, and the administrative staff. He had an effervescent personality — you could tell he was engaged, and he embraced a team approach.”
As chair of the RFS during the first year of his fellowship and then chair of the ACR Young and Early Career Professional Section (YPS) during his second year, Krishnaraj spent two years on the ACR Council Steering Committee (CSC). After hearing him speak about his fellowship research at a council retreat, Thrall and other key MGH leaders invited Krishnaraj to join the faculty full time. But there was a catch.
Since the abdominal imaging department was already fully staffed, the leaders urged Krishnaraj to apply for an academic career development grant to fund his salary for the first years of a five-year contract. With the grant application deadline just a few weeks away, Krishnaraj scrambled to complete the paperwork. He mentioned the dilemma to Mueller, who not only wrote a strong letter of recommendation but also released Krishnaraj from his clinical duties for two weeks to focus on the application.
With guidance from Zalis, who had received the same grant several years prior, Krishnaraj crafted a winning proposal. “It was truly a career-changing opportunity to have formalized mentorship through the grant application process and beyond,” Krishnaraj says. “The grant also provided additional funding to pursue more coursework, so I took classes in public health and computer science to shore up my foundational knowledge. These opportunities rounded out my education and focused my interests in the field of radiology.”
Young Leader
Krishnaraj had been on faculty at MGH for two years when his wife became pregnant with their second child. With a little girl on the way, he and Sarah began to look for opportunities to return to the South. “It started to dawn on us that we were spending a lot of time and money flying back and forth from Boston to North Carolina to see our families,” he says. “We knew that if an opportunity opened somewhere in the mid-Atlantic, we’d jump on it.”
Once again, that opportunity came through his ACR connections. At a CSC retreat in 2011, Krishnaraj had a conversation with Alan H. Matsumoto, MD, FACR, radiology department chair at the University of Virginia (UVA) Health System, who mentioned that the hospital’s thoracic-abdominal division director was planning to retire.
“Alan asked me if any faculty at MGH might be interested in the opportunity, and I jokingly said, ‘Gosh, if this was five or six years from now, that would be the perfect job for me,’” Krishnaraj recalls. A few months later at the ACR Annual Meeting, Matsumoto approached Krishnaraj again and encouraged him to consider the position — despite being 20 years younger than many of the department faculty.
“Even though he was relatively young and inexperienced in his career, Arun had already demonstrated that he was a highly engaging, emotionally mature person with good communication skills,” says Matsumoto, who was recently appointed vice chair of the BOC. “Since he had all the characteristics that we were looking for in a new division chief, I thought investing in him could help the department become better.”
In 2013, Krishnaraj and his family relocated to Charlottesville, just a few hours’ drive from their families in North Carolina, and he joined UVA as the head of the thoracic-abdominal division. However, that title soon changed as he began to transform the division.
“The structure of the division was a bit antiquated,” Krishnaraj explains. “By that time, most academic departments had separate cardio-thoracic or abdominal imaging sections, instead of blending them together. I wanted to effectively split the division into two different sections to be more congruent with other academic centers.”
Eventually, Krishnaraj became chief of the division of body imaging and chief of the abdominal imaging section while naming a separate thoracic section chief. Although there had been talks of splitting the division before his arrival, Krishnaraj brought the ability to build buy-in throughout the transition.
“That’s where his emotional maturity and communication skills kicked in,” Matsumoto says. “He understood that you can’t come in with guns a-blazing. Because of his ability to connect with everyone, he was able to navigate strong egos and differing opinions to implement a big change that allowed both areas to thrive and develop better subspecialty services.”
Lean Practice
As the body imaging division grew under this new structure, increasing volumes were causing delays for patients and long hours for radiology staff. To address these procedural backlogs, Krishnaraj enrolled in a class at UVA’s Darden School of Business that focused on operational efficiency. The course introduced him to the concept of Lean, a process improvement method traditionally used by automakers and manufacturers to streamline complex workflows by eliminating waste and redundancy.
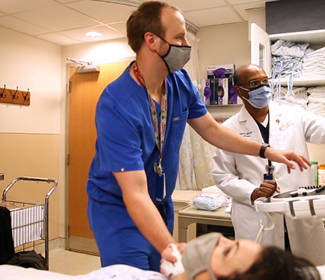
Krishnaraj is committed to patient-centered care and often goes out of his way to engage directly with patients alongside technologists and other care partners. |
Krishnaraj saw Lean improvement as a potential solution for the inefficiencies that plagued his division’s procedural service. His professor introduced him to former UVA student Austin English, a business consultant and visiting professor with experience implementing Lean practices.
“Arun was one of the first healthcare providers to ever call me,” says English, who typically consults with industrial clients. “It was refreshing to talk with a provider who recognized that some of the things they do in healthcare don’t make sense. He was open to looking beyond his silo to reimagine the processes they used.”
English and Krishnaraj examined the workflows involved in body imaging procedures, bringing together members from across the division, from scheduling to housekeeping, to discuss each person’s contributions to the process. Using Lean, they identified redundancies that could be eliminated to streamline the workflow.
“No one person does a procedure by themselves,” says Krishnaraj, who has been director of body procedures since 2015. “The nurses, the physicians, the techs, the schedulers, and the housekeeping staff all have to work in unison. Lean helped us understand the value that each team member provides so that we could optimize their contributions.”
With a few changes, like creating pre-procedure checklists and shuffling staff responsibilities, Krishnaraj transformed the efficiency of the body imaging procedural service to drastically reduce wait times — essentially doubling the procedure volume within a couple of years. English still uses the case study about this project to teach his business classes how to implement Lean.
“The way Arun applied Lean practices to streamline his division is a prime example of how even in healthcare, you have to keep evaluating every process if you want to deliver more value,” English says.
Patient Focus
As Krishnaraj continued to bolster his education, he also had plenty of opportunities to help educate others about the jargon and technical terms often used in radiology. He traces this role back to his residency, when Sarah’s uncle was diagnosed with colorectal cancer. Throughout the diagnosis and treatment process, the family often asked Krishnaraj to explain the imaging results and recommendations.
“Ever since I started medical school, people have gravitated toward me as a guide and a translator for health appointments and questions,” Krishnaraj says. “I realized that many healthcare providers struggled to explain procedures and conditions in ways that patients could under-stand, so people often left appointments feeling overwhelmed and confused. I felt a huge amount of frustration for what patients were experiencing in their healthcare encounters.”
Krishnaraj got the chance to start addressing some of these challenges on a broad scale in 2016, when James V. Rawson, MD, FACR, asked him to join the ACR’s newly formed Commission on Patient- and Family-Centered Care (PFCC). As co-chair of the PFCC Informatics Committee — with Tessa S. Cook, MD, PhD, the director of 3D and advanced imaging at Penn Medicine in Philadelphia — Krishnaraj explored ways to leverage technology to improve the patient experience.
When Rawson moved into a position on the BOC, Krishnaraj was elected as chair of the PFCC. “The main purpose of the PFCC is to provide resources to help physicians take better care of their patients to ensure the best experience possible,” he says. These resources include Radiol-ogyInfo.org, a website jointly funded by the ACR and the Radiological Society of North America (RSNA) that Krishnaraj has contributed to since 2012. He currently chairs the committee that manages the site, which garners nearly 2 million visitors a month.
While spearheading these national resources, Krishnaraj also rolled out smaller-scale initiatives at UVA that have served as models for patient-centered care. Ever since he started translating imaging results for his wife’s uncle, for example, Krishnaraj wanted to reimagine the standard radiology report to make it more engaging and visually appealing for patients.
Inspired by a 2010 Wired magazine contest to redesign the patient health record, Krishnaraj worked with Christina Swanson, MA, a graphic designer in UVA’s marketing department, to rethink their radiology report. Krishnaraj and Swanson added infographics and color-coded systems to illustrate difficult concepts like radiation exposure. They also inserted photos of the radiologists who read the reports and a contact number that referring physicians and patients could call with questions.
“We were among the first to include a hyperlink at the bottom of all our reports, linking to a short survey that basically asked, ‘How are we doing?’” Krishnaraj says. “The intent was to get feedback from our referring providers about our service levels, but surprisingly, three-fourths of the responses we get are from patients and their families. That feedback is extraordinarily valuable because it helps us understand how our reports inform someone’s view of their healthcare.”
Personal Connection
Krishnaraj’s patient-focused approach doesn’t end with radiology reports. He is also committed to connecting directly with patients and modeling patient-centered care in every interaction. For example, when a patient named George Beker requested clarification on a scan related to his cancer diagnosis, Krishnaraj sat down with him and his wife, Jeanna, to review the results and answer their questions.
“I like to have a lot of data, so it was really impressive that Dr. Krishnaraj spent the time with us to explain what he saw on my scans,” says George, a two-time cancer survivor who has been disease-free for eight years. Jeanna adds, “Although we were both emotionally distraught, he made the whole experience reassuring as well as educational. He’s a natural-born teacher who can articulate, in the clearest of terms, what he’s seeing and what it means. He saved us both many sleepless nights and a tremendous amount of stress.”
Through the years, as George and Jeanna returned to UVA for routine scans, Krishnaraj continued to treat them like VIPs — ensuring that they had access to imaging reports as soon as possible. “Waiting several days for a radiologist’s reading was horrible for me and caused anxiety,” George says. “Arun knew that, and he made sure that my exams were read right away. He took minutes out of his busy day to call me so I could rest easy. His responsiveness made my life much better.”
Over time, the Bekers got to know Krishnaraj personally as he regularly reached out to check on their health and ask about their work. Since then, the Bekers have hosted Krishnaraj and his wife for dinner several times and built a relationship beyond the hospital. “We now count him as a friend, not just an incredible medical resource,” Jeanna says.
While forging friendships with patients might not be the norm for radiologists, Krishnaraj says, “My connection with them is emblematic of the optimal way that I hope patients and radiologists can interact.”
To foster more of these connections, Krishnaraj actively engages on social media. It was on Twitter that Krishnaraj first met Amanda Crowell Itliong, a patient in Michigan living with ovarian cancer for the fourth time in 13 years.
“After a long, terrible day at the imaging center, where I ran into problems trying to get a CT scan, I went on Twitter and complained about it,” recalls Itliong, who’s navigated dozens of scans through the years. “Arun was frustrated to hear about my experience and got in touch with me. He ended up inviting me to get involved with the ACR, which offered me an opportunity to make meaning out of my struggles.”
After several conversations, Krishnaraj asked Itliong to share her perspective as a patient advocate with the PFCC. She joined the commission’s Patient Experience Committee in 2016 and became committee co-chair in 2021 — the first patient in the ACR’s history to serve as a chair.
“I never would have connected to the ACR in a million years if Arun hadn’t reached out to me on Twitter,” Itliong says. “He is one of those rare doctors who realizes they can never really know what it’s like to just be a patient. He’s always valued the expertise and insight that patients uniquely bring to the table, and he really listens to us because he genuinely wants to make healthcare better.”
Population Health
While the individual patient experience has been a driving force throughout Krishnaraj’s career, his background in public health has also prompted him to consider radiology’s broader role in healthcare.
“Radiologists have historically been single-episode providers rather than providing longitudinal care,” he says. “With the rise of breast cancer screening, CT colonography, and lung cancer screening, radiologists have gained a foothold in population health. Now, with the advent of artificial intelligence (AI) and machine learning algorithms, population health is far more than just those few screening modalities. Population health can take the form of all the incidental findings that a scan might reveal.”
To explore the population health potential of imaging, Krishnaraj is researching how machine learning can help document all imaging data for more comprehensive reporting. For example, if a patient gets a CT scan to diagnose abdominal pain, the scan also collects information about the fat content of their liver, the density of their bones, and the calcifications in their vessels — which, while perhaps unrelated to the diagnosis at hand, could be risk factors for other comorbidities.
“A lot of information isn’t being conveyed because it’s time-consuming for radiologists to note, but machine learning algorithms can rapidly and accurately gather and report this information,” Krishnaraj says. “AI will remove the cognitive burden of the tedious tasks that radiologists do every day — like counting pulmonary nodules or measuring the loss of vertebral body height — so that we can focus on a high-value experience with the best quality care. By leveraging this technology, radiologists can become vital to longitudinal primary care and population health.”
Krishnaraj also sees potential in screening healthy individuals as part of an annual physical exam to monitor changes in the body over time. He recently received an ACR grant to study the use of low-dose CT to scan participants before and after training for a 10K race in Charlottesville, using AI algorithms to evaluate changes in fat distribution. “This could open the door to people coming in to get routine low-dose imaging that will give us a complete picture of someone’s health using a variety of AI algorithms,” he says. “I’m very bullish on the future of imaging as a valuable aspect of patient care in an increasingly tech-centered world.”
Team Spirit
It’s not surprising that Krishnaraj has a strong vision for the profession. After all, the ability to imagine and execute toward a better future is a hallmark of a good leader. It’s one of the main characteristics that Krishnaraj idolized about UNC basketball coach Dean Smith. “He could inspire players to step up and execute in key moments,” says Krishnaraj, who had the chance to meet his childhood idol when he came into UNC for a scan. “What a powerfully important skill for a leader to have and hone, that ability to engage people in a way that motivates them to do something bigger than themselves.”

Krishnaraj has a close-knit family that includes his wife, Sarah, and his children, parents, and brother. |
Even though Krishnaraj didn’t get to fill Smith’s shoes, he is still fulfilling his coaching dreams. As UVA’s abdominal division leader and the president of his state ACR chapter, he mentors many residents and fellows in the development of patient-centered care innovations. “There’s great power and meaning in sharing your knowledge to help someone else,” he says. “The more time you give to mentor others, the more it gets paid back to you through a legacy that will outlive you.”
When he’s not working, Krishnaraj has found ways to live out his basketball dreams, too. He coaches his son’s youth basketball team, and he goes to the recreation center a few times a week to shoot hoops as part of a local league. His children inherited his love of sports, too. Both Nayan, age 11, and Priyanka, age 9, play basketball and tennis.
Instead of striving for balance between coaching his children and mentoring others, Krishnaraj tries to blend the two, including his family in his work whenever possible. For example, he and Sarah love to travel — they’ve visited 15 countries together and have more trips planned — so whenever professional society meetings or presentations take him out of town, Krishnaraj opts to bring his family along, if he can. But the blending doesn’t stop there. Krishnaraj often practices delivering his presentations in front of his children, and as a result, they both enjoy making presentations for school. Always the conversationalist, Nayan even enjoys talking with other radiologists when he gets a chance.
Krishnaraj hopes that his influence on students, residents, fellows, and, of course, his children will long outlive his medical career — leaving a legacy like that of Dean Smith. “At UNC, they talk about Dean Smith’s coaching tree in reference to the number of coaches he’s spawned and the players he’s coached who have gone on to accomplish even more,” Krishnaraj explains. “Being a physician gives you the opportunity to create a tree of your own, where you can look back on all the medical careers you’ve helped launch, and how they went on to help others. The broader your tree is, the more lives you’ve affected, and the fuller your contributions have been.”
Radiology’s Future
Krishnaraj admits, however, that success isn’t only measured by the size of your coaching tree. For him, it comes back to “improving the day-to-day experiences of patients and their families who are accessing the technological marvel that is imaging,” he says. “If my efforts help ensure that someone has a good experience with radiology, then I’ll feel proud that my career has been worth it.”
Not only is patient-centered care the most fulfilling aspect of medicine for Krishnaraj, but he believes it’s also critical to ensuring radiology’s relevance as AI evolves in the future. In order to survive, he says, radiologists must emerge from their reading rooms to directly engage with patients. That’s why he’s currently mentoring a resident to provide virtual consults for patients who want to have their imaging results explained.
“It’s fulfilling for both parties when we get to meet the person behind the black-and-white images on the screen,” Krishnaraj says. “This is the reason why we do what we do. When you pursue the calling to become a physician, it’s not just to generate reports for other doctors. It’s to make sure that those reports are accurate and meaningful for patients.”
That value, he says, cannot be easily replaced by machines. To prepare for further advancements in technology, Krishnaraj encourages radiologists to think beyond image interpretation and prioritize empathetic patient care. “If we put our entire value proposition on reading scans, then we’re playing a game that we can’t win because machines will eventually do that better than we can,” he says. “But if we focus on the human connection and providing the best possible care to each patient, then we’ll always have a role to play.”





