This article is the third in a five-part ACR Bulletin series and examines the role of mobile health screening in underserved communities. The second article in the series, A Health Equity Hurdle: Access to Affordable CT Colonography, was posted in September.
Efforts to eradicate disparities in delivering critical imaging services continue to gain momentum as systemic problems loom large over the house of medicine. Current healthcare inequities in radiology can result in lower quality of care, poor patient outcomes and higher costs to patients and providers.
Marginalized populations often face barriers to treatment — including education and outreach, access to healthcare services and a host of social determinants that plague underinsured and underserved communities. Initiatives that establish health equity partnerships and build from innovative institutional efforts to ensure equitable care on a united front are putting vital services within reach.
The ACR is part of the Radiology Health Equity Coalition (RHEC), a group of organizations that joined forces in 2021 to positively impact health equity for vulnerable outlier populations. To paint a picture of how radiologists and physicians from other specialties are moving the needle, the ACR Bulletin is interviewing changemakers who are striving to meet coalition goals around advancing equitable care.
Data-Driven Community Mobile Health Services
Underserved communities in both urban and rural areas face barriers to routine healthcare services that many individuals with insurance and more education on how to navigate the system for recommended screenings may take for granted. A group of physicians, working with partners in private industry and through local outreach programs, decided it was time to act. They hit the road with mobile health units (MHUs) to deliver services to marginalized populations in Detroit and surrounding counties — with eyes on expanding the fleet and the concept beyond Michigan’s borders.
To build out our concept of mobile CT screening quickly and at scale, we realized that we needed to move beyond academia.
“I’m an ER doctor by training, but I left the ER because I got tired of throwing Band-Aids on problems such as heart attacks or strokes that could have easily been prevented by better access to screening and more effective linkage to appropriate social services and medical care,” says Phillip D. Levy, MD, MPH, professor of emergency medicine and associate vice president of translational science at Wayne State University. He is also the director of the MHU program for Wayne Health, previously Wayne State University Physician Group.
Levy was frustrated with unnecessary barriers to self-elected screening for people who are marginalized by society and underserved from a healthcare perspective. “We taught people during COVID-19 that you can go to your local municipality or public health agency or a mobile unit and get a COVID-19 test without a prescription,” he says. “Why should we now put restrictions on basic healthcare and radiology services when they can be delivered in the same way?”
As many providers witnessed during COVID-19, outcomes were not driven entirely by the disease itself. They were largely influenced by social vulnerability.
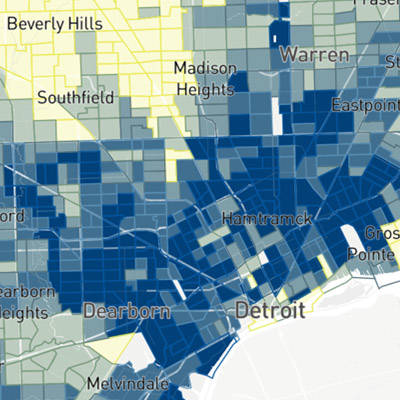
“Prior to the pandemic, we had started aggregating data such as blood pressures from emergency department encounters across the region and using geospatial analysis to identify where risk is greatest,” Levy says. “We developed the population health outcome and information exchange (PHOENIX), with the idea that we would have a running ticker of health-related information aggregated at a community level that, when tied in with upstream mediators and moderators, would help identify the predominant upstream factors that affect downstream health outcomes.”
The data allowed the group to identify communities with a high degree of social vulnerability, food insecurity, poor hypertension control and high cardiovascular event rates.
When the pandemic hit, Levy created the Wayne Health Mobile Unit (WHMU) program, with an initial goal of addressing COVID-19-related healthcare needs such as testing and, soon thereafter, vaccinations. Building on its successes, the WHMU program expanded to a vision of portable population health, adding blood pressure and other health screenings, as well as standardized social determinant assessments enabling provision of services to patients in more vulnerable populations throughout Detroit and surrounding communities.
"We thought that as long as we were already out in the communities, we should start to assess for social factors and create a comprehensive intake process that could help us identify and address social determinants,” Levy says. “Then we thought, if we’re going to do that, we should include patient health navigators and community health workers in the field who can link people to services. And while we’re at it, why don’t we start checking blood pressures and draw blood to look at cholesterol levels, check hemoglobin A1C concentrations, evaluate for kidney disease and so on. It was our vision to improve access for people whom we know are at high risk, neighborhood by neighborhood.”
Mobile Insite into Lung Health
New mobile efforts to reach vulnerable populations are now in play for lung cancer screening. “Detroit has some of the highest smoking rates in the country, especially amongst the Black population, ” Levy says. “Obviously that is very concerning from a lung cancer detection perspective — and lung cancer screening is grossly underutilized.”
Levy recognized early on during the COVID-19 screening phase that extending mobile screening services on a larger scale and beyond the borders of Michigan would require forming a private company. That idea gave birth to Mobile Insite. “The task at hand to develop the business was quite daunting, and we decided to partner with People.Health , a company that has existed for close to a decade with a mission of enhancing patient access to health-related information and services,” Levy says. Using the WHMU program as a predicate concept, Mobile Insite was formed as a subsidiary of People.Health.
“As we were conceptualizing this model, we realized that the right pathway for it was in the private sector,” Levy says. “From the health equity perspective, you really need to look beyond the typical currency of research papers and grants to how many people you can actually reach and serve in your community.”
To help the most people, it is important to meet them where they are, which is the magic of mobile screening. “This project is exciting, and we’re really passionate about removing barriers to routine healthcare,” says Donna M. Roussey, director of clinical operations for Mobile Insite. “We really want to get out into the communities to reach people for free lung screenings to detect nodules and potential cancer.”
Roussey has been active in radiology and imaging for more than two decades — serving as a CT technician, working with physician groups to develop scan protocols and workflow, helping outpatient centers improve imaging efficiency, and revamping the patient experience by streamlining imaging processes from scheduling through to follow-up recommendations.
Through her work, she knows there is a lengthy timeline from when a patient decides to see a doctor through to the office visit, scheduling a CT exam, getting the scan and then possibly going back in for follow-up procedures.
“Being mobile takes such challenges away,” Roussey says. “It takes the guesswork out of how to get patients through a lengthy process that they often don’t know how to start. Patients may know they are at risk for lung cancer due to many years of smoking, for instance, but they have no one to help them navigate the system. It can be pretty intimidating, and when you take the services to them, it can alleviate a lot of anxiety.”
Levy and Roussey intend to use specialized vans equipped with compact mobile low-dose cone beam CT scanners for screening in underserved populations that are at risk for lung pathology. To achieve this, they will have two vehicles, each about the size of an ambulance and equipped with a cone beam CT system developed by medical imaging solutions company iCRco, and will be using refined scanning protocols, Roussey says. Another partnering company, Surgical Training Institute, is outfitting each vehicle with the CT equipment, a small bump-out for a desk area and a lift to assist people in wheelchairs.
The vehicles will have proper radiation barrier walls and other safety equipment that meet the same requirements of facility-based radiology environments. They are expected to be finished this month, and the project is on track to roll out by the end of the year.
“We want to make sure we have everything in order before we launch,” Roussey says. “To make the process less time-consuming, this includes having forms and questionnaires ready and establishing the most efficient and effective flow of reading scans, delivering results to patients and facilitating next steps if findings indicate the need for other follow-up care.”
Mobile screening is an effective way to reach people in underserved communities to educate them on other aspects of their health — to get them invested in taking care of themselves. “We will provide our mobile CT screening for free, but we also want to do follow-up services so patients will know that we will help them navigate treatment for any suspicious findings,” Roussey says.
“So much of this is about building trust in a community,” Levy says. “We don’t want patients to feel like they are being commodified, so there will be no cost to the patient for this. We hope patients will see how committed we are to problems before they become life-threatening or irreversible.”
The Path to Funding and Partnerships
“Since the launch of the WHMU program, we have sent vehicles out to around 3,500 events — with six to eight vehicles going out into communities each day,” Levy says. “The receptivity to it has been tremendous, and we have similar high hopes for CT lung and other screenings.”
The success of any health equity effort depends in no small part on securing funding and building partnerships. “When we first started with the WHMU program, a lot of philanthropy came in to support us,” Levy says. “The Michigan Department of Health and Human Services also got behind the program, especially its Coronavirus Task Force on Racial Disparities, which was formed to better understand why Brown and Black communities were disproportionately affected by COVID-19 and develop effective interventions. Our MHU program became a pillar of that. Fast-forward a few years later, and we have a fleet of eight vehicles that have conducted nearly 90,000 encounters with almost $60 million in funding from various sources.”
Some funding has come from National Institute on Minority Health and Health Disparities grants, and other support from the American Heart Association and corporate donations. “We have also been in talks with the RHEC and the Michigan Radiological Society to gain their endorsement for community screening to enhance health equity,” Levy says.
The program is working with the largest Medicaid managed care organization in Wayne County to reach more people who are not engaging in healthcare services. “We have geolocated these people and are working with the insurer to deploy vehicles in communities with a high density of untreated individuals,” Levy says. “The insurer is paying us using a new billing code we created with them to enable MHU-based delivery of place-based bundled prevention screening services.”
In the future, Levy would like to see this move from blood pressure and diabetes evaluation to include the new mobile CT screening for lung nodules and eventually blood biopsies along with coronary calcium and structural heart disease detection.
“We run local television and radio commercials to get the word out on existing mobile screening programs and will continue to do that for expanded services,” Levy says. This type of messaging — in tandem with building local faith-based, public health and community center partnerships — is powerful and effective, he says. Strengthening relationships with area providers is also critical so there can be a seamless transition in making images available to providers and their patients.
“The ACR obviously wants radiologists and the specialty as a whole to play a big role in health equity,” Levy says. “In line with the College, we want to show how you can reach the masses — with radiologists facilitating imaging interpretation, but without having to be the inlet to services.”
The current healthcare delivery system is not adequate or fair, Levy says. “If we expect it to work as is — with patients scheduling an appointment that could take months to get and then self-selecting follow-up care after a scan — we will continue to see unnecessary delays and patient frustration around screening.”
It can be an uphill battle. “Some people don’t want to know,” Levy says. “They get nervous. They don’t want to know what they have because then it becomes something they have to deal with.”
However, education and ease of access can translate into clinically functional models of health equity, he says.
“The real value from a health equity perspective is not how many scans you bill for, but how much disease you can identify and how easily you can link folks to the next appropriate level of service,” Levy says. “We are not the only ones who can do this, and we hope others will take a closer look at what we are accomplishing. Our ethos is all about reaching and serving more people. If our model can be more widely promulgated, the better off society will be.”
To Learn More
More information about the WHMU program is available here.